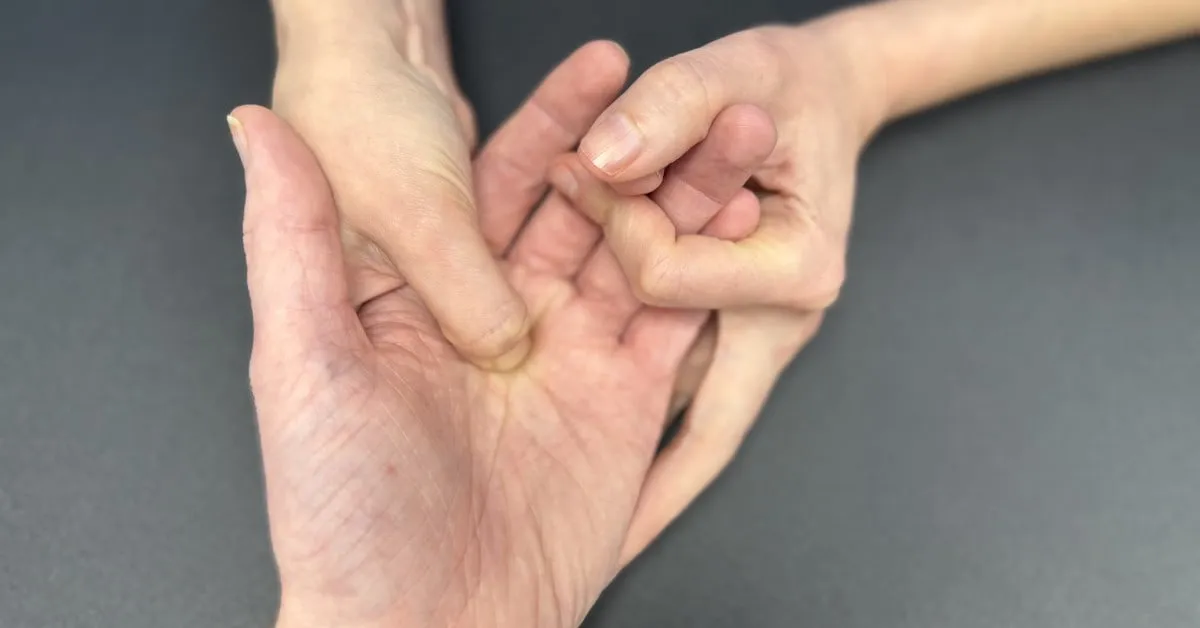
Trigger finger, known medically as stenosing tenosynovitis, is a condition in which a finger or thumb becomes caught or locked in a bent position. It produces a characteristic clicking or snapping sensation when you try to straighten it. The condition can affect any finger and when it involves the thumb it is called trigger thumb. Trigger finger is more common than many people realise. It tends to affect people between the ages of 40 and 60, is more common in women and is associated with conditions such as diabetes and rheumatoid arthritis. If you have noticed clicking, locking or pain at the base of a finger, you may be experiencing trigger finger.
-
Yes. Hand Therapy can often resolve trigger finger and trigger thumb without injections, particularly when treatment is started early. A structured programme of splinting, specific exercises and activity modification is effective for many patients across Grades 1 to 3. Ms Razo's approach focuses on non-operative management first, with corticosteroid injections considered only if Hand Therapy has not achieved sufficient improvement.
-
A corticosteroid injection may be considered when Hand Therapy alone has not fully resolved the triggering, or where the severity of symptoms makes early injection appropriate. If an injection is the right option, Ms Razo can refer for an ultrasound-guided injection at a private independent clinic. Ultrasound guidance improves accuracy and is preferable to a blind injection.
-
Trigger finger and trigger thumb are progressive conditions. Without treatment, most cases will advance through the grades of severity over time. A finger or thumb that catches or clicks today may become locked and painful if left untreated. In advanced cases, the digit can develop a fixed flexion contracture where it cannot be straightened even with assistance. Early treatment is associated with better outcomes and a reduced likelihood of requiring surgery.
-
Spontaneous resolution is uncommon. Mild symptoms may settle temporarily with rest, but triggering typically persists or progresses without structured treatment. Splinting and Hand Therapy are effective non-operative options that can resolve triggering in many cases when started early.
-
No. Trigger finger and trigger thumb are tendon conditions, not joint conditions. They occur when the A1 pulley at the base of the digit becomes thickened and inflamed, restricting tendon gliding. However, triggering is more common in people with rheumatoid arthritis and other inflammatory conditions. If you have both trigger finger or trigger thumb and joint symptoms, a specialist assessment can determine whether one or both are contributing to your problem.
-
The medical name for trigger finger is stenosing tenosynovitis. Stenosis refers to a narrowing and tenosynovitis refers to inflammation of the tendon sheath. When the condition affects the thumb it is called trigger thumb, but the underlying mechanism is the same.
-
Yes. Trigger thumb involves the same mechanism as trigger finger. The A1 pulley at the base of the thumb becomes thickened and inflamed, causing the tendon to catch or lock. The same grading system applies and the same non-operative treatment approach is used. Trigger thumb can sometimes feel different because the thumb plays a more prominent role in grip and pinch, meaning symptoms can affect daily activities more noticeably.
-
Safe activities include warm water immersion before gentle movement, passive stretching of the affected digit and specific tendon gliding exercises. The exact movements, frequency and duration should be prescribed by your Hand Therapist based on your grade of triggering. Exercises that involve resisted gripping, stress balls or grip strengtheners should be avoided as they can aggravate the A1 pulley inflammation and worsen the condition.
-
Stress does not directly cause trigger finger or trigger thumb. However, sustained or repetitive gripping under tension, including stress-related hand clenching, can contribute to overuse of the flexor tendons and increased friction at the A1 pulley. If you notice that your symptoms worsen during periods of stress, it may be worth considering whether habitual gripping or clenching is a contributing factor.
-
Recovery depends on the grade of triggering and how early treatment begins. Many patients with Grade 1 or 2 triggering see a significant reduction in symptoms over a prescribed period of consistent splinting and activity modification. More advanced grades may require a longer treatment programme. Your Hand Therapist will give you a realistic assessment of what to expect at your initial appointment.
How does trigger finger happen?
To understand trigger finger, it helps to know a little about how the tendons of the hand work. The flexor tendons run from the forearm through the palm and into the digits, allowing you to bend your thumb, fingers and grip. These tendons pass through a series of tunnels called tendon sheaths and are held close to the bones by tight bands called pulleys.
In trigger finger and trigger thumb, the A1 pulley, which sits along the base of the digit at the level of the palm, becomes thickened and inflamed. As the tendon passes through this narrowed section, friction builds up and a small nodule often forms on the tendon itself. The nodule catches on the pulley when the finger is straightened, producing the triggering effect. In more severe cases, the finger or thumb can become locked in a bent position and cannot be straightened without using the other hand.
Trigger finger and trigger thumb can develop without any obvious cause, but contributing factors include:
- Repetitive gripping activities: manual work, gardening or sports involving sustained gripping.
- Diabetes: significantly increases the risk and can sometimes affect multiple digits.
- Rheumatoid arthritis: inflammation can affect the tendon sheath.
- Hypothyroidism: associated with tendon changes.
- Previous hand injury: particularly injuries to the palm, finger or thumb base.
- Sustained gripping or clenching: including stress-related hand tension, which can increase friction at the A1 pulley over time.
What are the symptoms?
Symptoms of trigger finger and trigger thumb typically develop gradually and may include:
- Pain or tenderness at the base of the affected digit, particularly in the palm.
- A palpable nodule: a small lump felt in the palm at the base of the affected digit.
- Catching or clicking: a snapping sensation when bending or straightening the digit.
- Stiffness, particularly in the morning or after periods of inactivity.
- Locking: the digit becomes stuck in a bent position and requires the other hand to straighten it.
- Swelling throughout the affected digit or specific joints.
The four grades of trigger finger
Trigger finger and trigger thumb are classified into four grades of severity, which guide treatment decisions:
- Grade 1 — Intermittent catching: pain and tenderness at the base of the finger or thumb in the palm. You may have a history of the digit catching, but it does not trigger during examination.
- Grade 2 — Active triggering: the finger or thumb visibly catches or clicks when you bend and straighten it, but you can straighten it on your own.
- Grade 3 — Locking: the finger or thumb locks in a bent position and cannot be straightened without using your other hand to push it back.
- Grade 4 — Fixed contracture: the finger or thumb is permanently locked in a bent position and cannot be straightened even with assistance.
Most people seek treatment at Grades 2 or 3. Grades 1 to 3 typically respond well to Hand Therapy including splinting and activity modification. Waiting until Grade 4 can make treatment more complex as a fixed contracture may require surgical intervention.
Will trigger finger get worse without treatment?
Trigger finger and trigger thumb are not dangerous conditions, but they are progressive without treatment. Most cases will advance through the grades over time and spontaneous resolution is uncommon. A finger that catches and clicks today may become locked and painful if left untreated.
Early treatment is associated with better outcomes and a reduced likelihood of requiring surgery. If you have noticed symptoms of trigger finger or trigger thumb, an early assessment with a Hand Therapist is advisable.
What are the treatment options?
Hand Therapy and non-operative treatment
Non-operative management without surgery is effective for many cases of trigger finger, particularly at Grades 1, 2 and 3.
Splinting is a cornerstone of non-operative trigger finger and trigger thumb management. A splint holds the affected finger or thumb in a specific position to prevent the triggering movement, allowing the inflamed pulley to settle. The type of splint used and which joint it immobilises depends on the digit affected and the grade of triggering. Ms Razo fabricates bespoke thermoplastic orthoses to precisely match each patient’s anatomy and presentation.
Activity modification is an important part of management. This means identifying and temporarily reducing the activities that provoke symptoms. It does not mean stopping all hand use, but making thoughtful adjustments to how and when you use the affected hand.
Not all exercise is appropriate for trigger finger or trigger thumb. High-repetition active exercises and gripping tools such as stress balls or grip strengtheners should be avoided as they can aggravate the A1 pulley inflammation and worsen the condition.
Safe activities include warm water immersion before gentle movement, passive stretching of the affected digit and specific tendon gliding exercises. The exact movements, frequency and duration should be prescribed by your Hand Therapist based on your grade of triggering.
Corticosteroid injection
Patients with trigger finger or trigger thumb are sometimes offered a steroid injection as a first-line treatment. Hand Therapy can often resolve trigger finger or trigger thumb without injections, particularly when started early. Ms Razo’s approach focuses on accurate differential diagnosis and non-operative management first.
If Hand Therapy is unsuccessful and a corticosteroid injection may be the right option. Ms Razo can refer for an ultrasound-guided injection at a private independent clinic.
Surgery
For cases that have not responded to non-operative treatment, or for Grade 4 fixed contractures, surgical release is the definitive treatment. The procedure involves dividing the A1 pulley under local anaesthetic, allowing the tendon to glide freely. It is a day-case procedure with generally excellent outcomes.
Post-surgical Hand Therapy is important to restore full movement, strength and function for optimising outcomes following the operation.
Trigger finger versus Dupuytren’s contracture
Both trigger finger and Dupuytren’s contracture can cause the finger to bend towards the palm and both produce a nodule that can be felt in the palm. They are, however, distinct conditions.
The key difference is that trigger finger involves catching, clicking or locking. The finger or thumb can usually be straightened (at least in earlier grades) but does so with a snap or jolt. Dupuytren’s contracture, by contrast, causes a gradual progressive tightening of the tissue beneath the skin, drawing the finger or thumb into a fixed bent position without any clicking or triggering.
In advanced trigger finger (Grade 4), a fixed contracture may closely resemble Dupuytren’s contracture. If you are unsure which condition you have, a specialist assessment will clarify the diagnosis.
Trigger finger and trigger thumb are also sometimes mistaken for arthritis because both cause pain and stiffness in the digits. However, triggering is a tendon condition affecting the A1 pulley, not a joint condition. The hallmark difference is the catching or locking sensation, which is not a feature of arthritis. Rheumatoid arthritis is a risk factor for developing trigger finger and the two conditions can occur together.
Trigger finger and trigger thumb treatment in Belfast
Ms Razo specialises in the non-operative management of trigger finger and trigger thumb, offering:
- Custom, thermoplastic splint fabrication and fitting
- A guided exercise programme tailored to your grade of triggering
- Activity modification and advice on protecting the pulley during recovery
- Education on what to avoid and why
- Post-injection and post-surgical rehabilitation
If you have noticed clicking, catching or locking in a finger or thumb, early assessment is the best step. Ms Razo offers prompt appointments with no waiting list. Book a consultation or contact the clinic to discuss your symptoms.